Treatments (Skin Care)
Beautify Enhance Renew
Healthy Skin Starts Here!
Your skin is the window to your body that reveals the stories of your life. From acne breakouts during your teenage years to the radiant glow of pregnancy and the sunspots of aging, both your age and your health are reflected in your skin. Call Dr. Grazer office in Newport Beach to learn more about our special skin care treatments.
Schedule Your Consultation with our Aesthetician Denise Stanek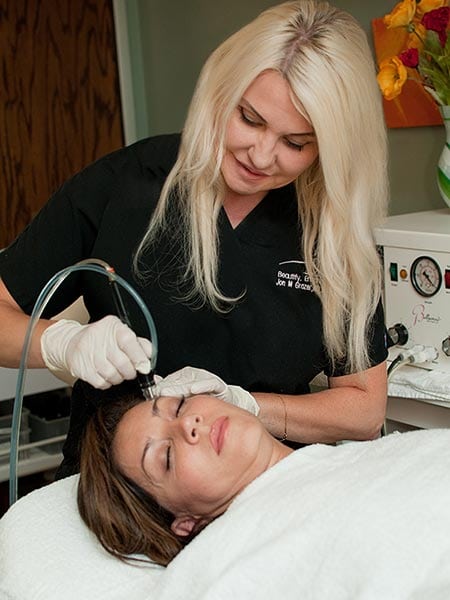
Using the finest high-grade ingredients and the newest, cutting-edge technology, we are dedicated to helping patients attain the most vibrant, youthful skin possible.
Medical Aesthetic Treatments
“Skin Quencher”
Dermal Infusion
Hydrate your thirsty skin as it is cleansed and exfoliated via our dermal infusion machine. DERMALINFUSION® is a patented, non-invasive, 3-in-1 dermatological treatment that simultaneously exfoliates, extracts, and infuses skin with condition-specific serums for an all-inclusive treatment in one step.
“Oxygenate to Rejuvenate”
Oxygen Facial
An infusion of oxygen (under hyperbaric pressure) and antioxidant serums leaves your skin radiant and hydrated. This extraordinary treatment smoothes fine lines, plumps up your lips and has a firming & tightening effect on your entire complexion. Also, perfect for acne patients due to oxygen s antibacterial effect.
* We recommend a series of six treatments for optimal results.
“Wrinkle Relaxer”
Atoxelene Facial
Atoxelene is a dermal relaxant made with natural amino acids and acts as skin smoothing complex. Relaxes fine lines and gives an “instant lift” to the skin. It can help prolong the effects of Botox, perfect before a night on the town!
Combination Rescue DUO
This treatment combines Oxygen & Atoxelene together for the ultimate rescue – resulting in beautiful skin perfect for a special event or just the envy of your friends!
“Time Blaster!”
Microdermabrasion
Microdermabrasion is a skin resurfacing treatment that uses crystals to gently exfoliate the top layer of skin. Microdermabrasion will leave your skin radiant and rejuvenated with no downtime.
This treatment helps minimize:
— fine lines & wrinkles
— enlarged pores
— acne & acne scarring
— sun damage/age spot
— uneven skin tone & texture
This 50-minute treatment includes cleansing, steam, calming mask and extractions.
“So Long Peach Fuzz!”
Biomedic Micropeel – (The Lunchtime Peel)
This unique treatment involves a 3 step process that involves Dermaplaning, which removes a micro-thin layer of skin and facial hair (Peachfuzz), a light chemical peel and finishes with a high-frequency treatment which kills bacteria and calms the skin
“Pimples -B- Gone”
Deep Pore Cleansing Acne Facial
This facial is ideal for anyone with clogged pores, occasional breakouts or acne. A gentle papaya bromelain enzyme is applied followed by steam for 10 minutes after which extractions are performed. Tea tree compresses are applied for anti-inflammation followed by a deep cleansing purifying clay mask. We finish this treatment with a high-frequency treatment that kills bacteria and helps blemishes heal faster.
“Complexion Jolt!”
Glycolic Acid Facial
Glycolic is an alpha-hydroxy acid peel that helps stimulate cellular turnover improving the overall radiance of the skin. Perfect for anti-aging, tired dull complexions and for treating acne conditions. Skin is cleansed, steamed and extracted, chemically exfoliated with the glycolic peel, and calmed with a cooling gel mask.
“VI peel”
VI peel is a chemical peel that not only helps to reverse sun damage and aging but also helps reduce melasma and or acne conditions.
This peel has little downtime, yet produces dramatic results in just days!
“Walk This Way … “
Back Facial
A back facial is perfect for anyone who has bumpy skin or breakouts on their back. This treatment includes steam and extractions covering the shoulders and entire back. A clarifying clay mask is then applied for withdrawing impurities and removing clogged pores.
“Out with the Toxins!”
Lymphatic Drainage
The lymphatic treatment is highly detoxifying and recommended for clients post facelift to help ease swelling and accelerate healing. A 15-minute massage with mild pumping movements is followed by a soothing gel mask.
“Light Stim”
LED infra-red light therapy firms and tightens the skin, reduces the appearance of pores, smoothes texture, and reduces the appearance of fine lines and wrinkles. Add to any facial.
“Micro-needle Treatment”
This treatment uses micro-needle technology to allow products to penetrate deep into the skin. Deep delivery of the products stimulates new collagen and elastin reducing the appearance of fine lines and improving skin texture. Can be used with hyaluronic acid, stem cells or platelet-rich plasma.
(Price is based on a selection of product.)
(May be 1- 3 days of mild pinkness depending on the depth of treatment.)
(Recommend skin numbing prior to treatment)
SCULPLLA H2 Mask & Serum
(Facial Filler Linke Results, Without a Needle)
We’re excited to introduce you to the pain-free, needle-free way to more beautiful skin!
— Pain-Free and Needle-Free
— Reduces fine lines and wrinkles
— Tightens and lifts the skin
— Stimulates collagen growth
— Improves skin tone
— Brightens and lightens skin
— Long lasting
Sculplla-H2 is the first non-injectable formulation of Poly-L-Lactic acid. The Poly-L-Lactic is combined with a unique hydrogen sheet mask, that when combined together creates a powerful delivery system for optimal infusion of these ingredients deep into the skin.
Why use needles when you can use Sculplla-HR, a safe non-injection treatment that stimulates your skin to make its own collagen, giving you firmer, tighter, smoother skin?
Collagen stimulation continues for 6 weeks after a single treatment and for 6 months after a series of 5 treatments done 1 week apart. Continue touch-up treatments as needed.
This treatment can be done as a stand-alone treatment or added on to almost any facial. So, say no to needles, and say yes to beautiful, smooth, firm, and plump skin the more natural way.
A la Cart Treatments
(Can be done alone or added to other treatments)
Glycolic/Lactic Acid Booster peel
These booster peels are a quick way to enliven any complexion. A nice finish to a microdermabrasion or facial
“Oh My Gounrde!”
Nourishing Pumpkin Enzyme Facial
Indulge your senses with this aromatic conditioning facial that is highly nourishing for the skin. It includes a pumpkin exfoliating scrub, a pumpkin enzyme that has over 100 nutrients, a pumpkin shea butter massage and finishes with a hydrating mask.
“Saving Face!”
Vitamin C Facial
Give your complexion a vitamin boost with this anti-oxidant treatment. This facial includes cleansing, steam & extractions, Vitamin C serums, followed by a shea butter relaxing massage. A tightening & firming mask completes this anti-aging facial. Perfect for lackluster complexions or just to slow down Father time.
“The Ruby Gem!”
Cherry Burst Enzyme Facial
After this facial, your skin will be radiant and glowing. This sister treatment to the Pumpkin Facial rejuvenates lifeless complexions and stirs up the senses with its wonderful cherry aroma. This includes a cherry exfoliating scrub, a cherry enzyme with steam, facial massage and a customized mask.
*Emergency Zit Zapper
with High Frequency
Wake up this morning with a breakout? Have something important tomorrow? Come in and get zapped! This oscillating current warms the blemish killing bacteria below. Soothes and heals blemishes faster! 5 minute
Soothing Eye Treatment (mask)
A soothing serum followed by an eye mask helps hydrate the delicate eye area. A nice compliment to any treatment
Cancellations, No Shows and Late Arrivals
In order to remain on schedule for all our clients in Newport Beach, we must shorten your treatment time if you are late for your appointment. The normal fee for treatment will remain the same.
Our appointment policies are meant to allow for more efficient scheduling of your service while assuring you are taken care of in a timely manner.
We ask that a 24-hour notice is given for cancellations, otherwise, a cancellation fee of $75.00 will be charged.
Thank you for your consideration.

